Venous Insufficiency
What is chronic venous insufficiency?
Arteries bring oxygen-rich blood from your heart to the rest of your body and veins return oxygen-poor blood back to your heart. When your leg veins cannot pump enough blood back to your heart, you have chronic venous insufficiency (CVI). CVI is also sometimes called chronic venous disease, or CVD. You have three kinds of veins: superficial veins, which lie close to the skin, deep veins, which lie in groups of muscles, and perforating veins, which connect the superficial to the deep veins. Deep veins lead to the vena cava, your body's largest vein, which runs directly to your heart.
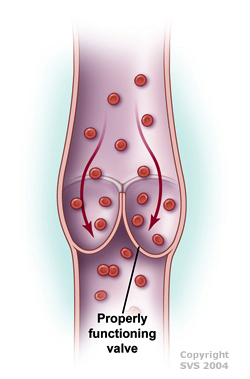
When you are in the upright position, the blood in your leg veins must go against gravity to return to your heart. To accomplish this, your leg muscles squeeze the deep veins of your legs and feet to help move blood back to your heart. One-way flaps, called valves, in your veins keep blood flowing in the right direction. When your leg muscles relax, the valves inside your veins close. This prevents blood from flowing in reverse, back down the legs. The entire process of sending blood back to the heart is called the venous pump.
When you walk and your leg muscles squeeze, the venous pump works well. But when you sit or stand, especially for a long time, the blood in your leg veins can pool and increase the venous blood pressure. Deep veins and perforating veins are usually able to withstand short periods of increased pressures. However, sitting or standing for a long time can stretch vein walls because they are flexible. Over time, in susceptible individuals, this can weaken the walls of the veins and damage the vein valves, causing CVI.
What are the symptoms?
If you have CVI, your ankles may swell and your calves may feel tight. Your legs may also feel heavy, tired, restless, or achy. You may feel pain while walking or shortly after stopping.
CVI may be associated with varicose veins. Varicose veins are swollen veins that you can see through the skin. They often look blue, bulging, and twisted. Large varicose veins can lead to skin changes like rashes, redness, and sores.
CVI can also cause problems with leg swelling because of the pressure of the blood pooling in the veins. Your lymphatic system may also produce fluid, called lymph, to compensate for CVI. Your leg tissues may then absorb some of this fluid, which can increase the tendency for your legs to swell. In severe cases, CVI and the leg swelling can cause ulcers to form on the lower parts of the leg.
What causes CVI?
Over the long-term, blood pressure that is higher than normal inside your leg veins causes CVI. This can lead to damage to the valves, which can further worsen the problem. In some instances, the valves that prevent blood from flowing “backwards,” can be congenitally defective. Other causes of CVI include deep vein thrombosis (DVT) and phlebitis, both of which cause elevated pressure in your veins by obstructing the free flow of blood through the veins.
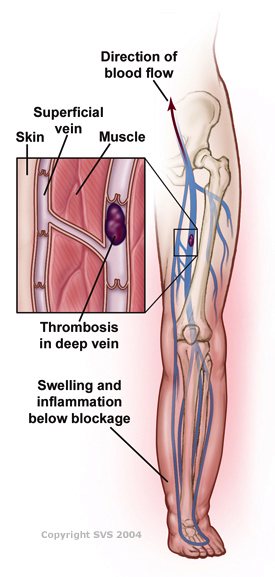
DVT occurs when a blood clot (properly called a thrombus) blocks blood from flowing toward the heart, out of a deep or perforating vein. The blood trying to pass through the blocked veins can increase the blood pressure in the vein, which, in turn, overloads your valves. Vein valves that do not work properly are called incompetent because they stretch and no longer work efficiently, and incompetent valves contribute to CVI. DVT is a potentially serious condition that causes leg swelling and requires immediate medical attention because sometimes the blood clots in the veins can break off and travel to the lungs. This condition is called a pulmonary embolus.
Phlebitis occurs when a superficial or deep vein becomes swollen and inflamed. This inflammation causes a blood clot to form, which can also lead to DVT.
Factors that can increase your risk for CVI include a family history of varicose veins, being overweight, being pregnant, not exercising enough, smoking, and standing or sitting for long periods of time. Although CVI can affect anyone, your age and sex can also be factors that may increase your tendency to develop CVI; women older than 50 most often get CVI.
What tests will I need?
First your physician asks you questions about your current general health, past medical history, and symptoms. In addition, your physician conducts a physical exam. Together these are known as a patient history and exam. Your physician may measure the blood pressure in your legs and will examine the varicose veins. To confirm a diagnosis of CVI, the physician may order a duplex ultrasound test or sometimes another test called a venogram.
Duplex ultrasound uses painless sound waves higher than human hearing can detect. Duplex ultrasound allows your physician to measure the speed of blood flow and to see the structure of your leg veins.
A venogram is an x-ray that also allows your physician to see the anatomy of your veins. During this test, your physician injects a dye, properly called contrast, which makes the blood in your veins appear on an x-ray.
How is CVI treated?
CVI is usually not considered a serious health risk. Your physician will focus his or her treatment on decreasing your pain and disability.
Compression stockings
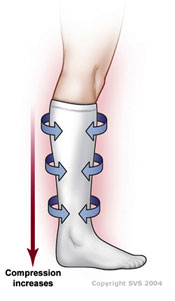
For mild cases of CVI, your physician may recommend compression stockings. Compression stockings are elastic stockings that squeeze your veins and stop excess blood from flowing backward. In this way, compression stockings can often also help heal skin sores and prevent them from returning. You may need to wear compression stockings daily for the rest of your life.
You can help avoid leg swelling and other symptoms by occasionally raising your legs and avoiding standing for long periods of time to decrease the pressure in the veins. When you do need to stand for a long period, you can flex your leg muscles occasionally to keep the blood flowing. You can also help lessen the symptoms of CVI by maintaining your ideal body weight or losing weight if you are overweight.
More serious cases of CVI may be treated with injections, called sclerotherapy, or with surgical procedures. Fewer than 10 percent of people with CVI require surgery to correct the problem. Surgical treatments include ablation, vein stripping, bypass surgery, valve repair, and angioplasty or stenting of a vein.
Sclerotherapy
In sclerotherapy, your physician injects a chemical into your affected veins. The chemical scars your veins from the inside out so your abnormal veins can then no longer fill with blood. Blood that would normally return to the heart through these veins returns to the heart through other veins. Your body will eventually absorb the veins that received the injection.
Ablation
Ablation uses a thin, flexible tube called a catheter inserted into a varicose vein. Tiny electrodes at the tip of the catheter heat the walls of your varicose vein and destroy the vein tissue. As with chemical sclerotherapy, your varicose vein is then no longer able to carry blood, and it is eventually absorbed by your body.
Vein stripping
To perform vein stripping, your physician first makes a small incision in the groin area and usually another incision in your calf below the knee. Then your physician disconnects and ties off all veins associated with the saphenous vein, the main superficial vein in your leg. Your physician then removes this vein from your leg. A procedure called ambulatory phlebectomy, or small incision avulsion, can be done either alone or together with vein stripping. Small incision avulsion allows your physician to remove individual varicose vein clusters from the leg through tiny incisions.
Bypass
For more extensive problems, your surgeon may recommend bypass surgery to treat CVI that occurs in the upper thigh or pelvis. For example, your surgeon can connect an artificial vein, called a graft, or a transplanted vein to a vein not affected by CVI to help blood flow from your affected leg around the blocked vein. Most vein surgery can be performed through small incisions. Usually bypass surgery is safe, although there is a small risk of DVT and infection at incision points. Your physician will only recommend this procedure in the most serious instances.
Valve repair
In valve repair, your surgeon shortens the valves inside your vein to improve valve function. After making a small incision into your skin, your surgeon cuts into the affected vein. Your surgeon then folds or tucks the valve flaps. He or she may place a fabric sleeve around the outside of your affected vein to help press the walls of the vein together to maintain valve function.
Angioplasty and Stenting
In more severe cases of CVI, your surgeon may recommend angioplasty or stenting. An angioplasty is the use of a balloon to push open a narrowed or blocked portion of the vein. A stent is a metal-scaffold tube that helps to keep the narrowed areas open. In some instances, depending on where the vein blockage is, this may be used to open up the blockage. The procedure is performed through small needle punctures in the veins, either behind the knee or in the groin. Typically angioplasty and stenting are safe procedures.
Your vascular surgeon will help you decide the best treatment option for your particular situation.

